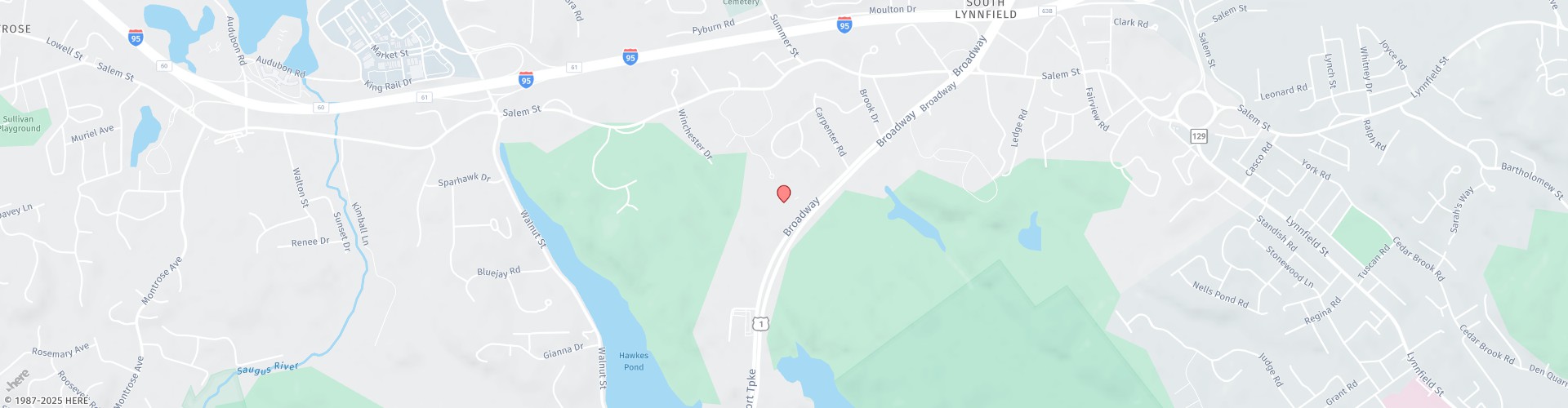
Normal Breast Thermogram
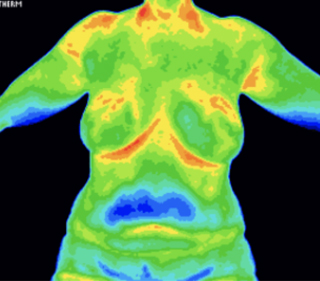
Abnormal Breast Thermogram
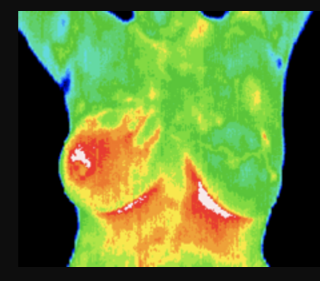
Breast Cancer Screening using breast thermography and breast imaging
At Optimal Wellness MD, we recognize the importance of regular screening for breast cancer in all women and in particular those women who have a higher personal risk or family history. Breast imaging is part of our evaluation of women who are contemplating hormone replacement therapy. We recommend using mammography, MRI, ultrasound, and thermography as appropriate.
Reference
Conclusion
“Thermography does not provide information on the morphological characteristics of the breast, but it does provide functional information on thermal and vascular conditions of the tissue. These functional changes are hypothesized to change before the onset of structural changes that occur in a diseased or cancerous state. It is known that physiological changes in tissue precede pathological changes,and studies support thermography’s potential role in the early detection of breast abnormalities that may lead to cancer. Since the late 1970s there have been a number of studies that have tested the effectiveness of this modality. If abnormal, thermograms are early indicators of functional abnormalities that lead to breast cancer, then there may be opportunities for early intervention to reverse the abnormal function toward normal. There is no one screening tool currently available that provides 100% predictability of the presence of a cancerous tumor. The only definitive diagnostic tool is a biopsy. In the past 30 years there have been numerous studies that have demonstrated thermography to have the ability to detect breast abnormalities that other screening methods may not have identified. The Ville Marie study demonstrated that thermography alone had a sensitivity of 83% in detecting breast cancer, while the combination of mammography and thermography had a 95% sensitivity. In light of developments in computer technology, and the maturation of the thermographic industry, additional research is required to confirm and/or continue to develop the potential of this technology to provide effective noninvasive early detection of breast cancer.”